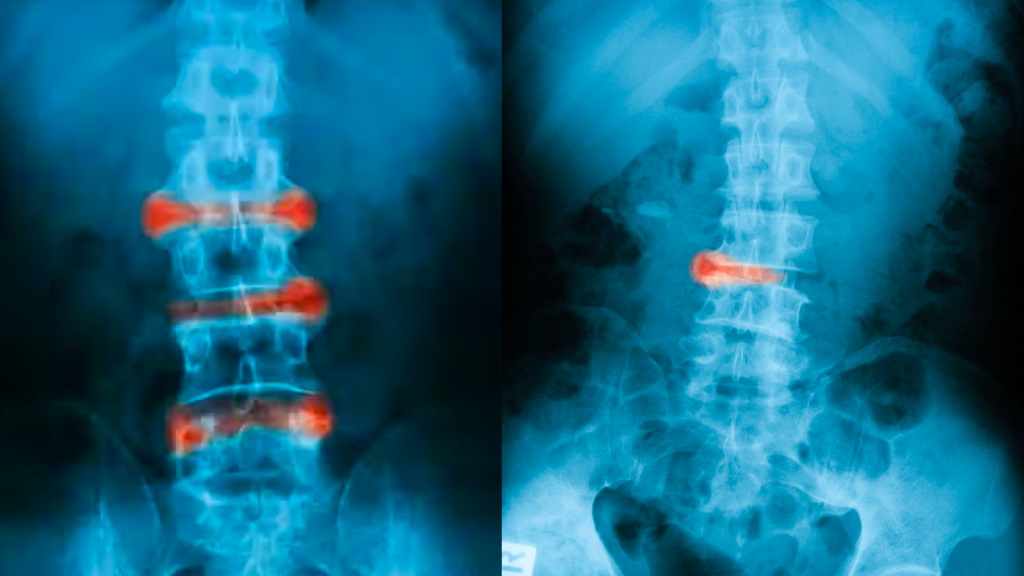
What is axial spondyloarthritis?
Axial spondyloarthritis is a chronic inflammatory disease that encompasses radiographic/ankylosing spondylitis (AS) and non-radiographic forms (nr-axSpA). Axial simply means the part of the skeleton that includes the spine and sacroiliac joints – joints that link the pelvis and lower spine. Non-radiographic indicates no visible damage on x-rays.
Ankylosing spondylitis (AS) is one of the most common types of inflammatory arthritis. Over time, it can cause some of the bones in the spine (vertebrae) to fuse. This fusing makes the spine less flexible and can result in a hunched posture or difficulty breathing when the rib cage is affected. AS affects approximately 1% of the population. It can strike at any age but is most common in people between ages 15 and 40. Almost all patients develop symptoms of back pain before age 45.
The main symptoms of axial spondyloarthritis
Ankylosing spondylarthritis primarily affects the spine, but can also involve the hips, knees, shoulders, and rib cage. The most common symptom is long-term back pain, along with spinal stiffness in the morning or after a long period of rest for both radiographic and non-radiographic.
Ankylosing spondylarthritis often presents differently in male and female patients. For instance, males have greater radiographic progression (as seen on x-ray) of the lumbar spine. Whereas female patients often present with associated conditions such as psoriasis or inflammatory bowel disease4. It is also important to note that female patients tend to have a high disease burden, in part because they have a longer delay in diagnosis, higher disease activity, and are significantly less responsiveness to treatment.
Ankylosing spondylitis is often mis-diagnosed as ordinary "low back pain" due to the common presentation. On the other hand, nr-axSpA is often misdiagnosed as fibromyalgia due to poor awareness and no visible change on x-ray.
Treatment of axial spondyloarthritis
Once a rheumatologist has diagnosed axial spondyloarthritis, there are effective treatments available to help manage symptoms and minimize joint damage. While there is no known cure, treatments are available.
Medication treatments include COX-2 inhibitors, glucocorticoid, traditional disease-modifying anti-rheumatic drugs (DMARDs), and biologic DMARDs. These medications can work alone or frequently, in combination, to reduce the pain and other symptoms associated with ankylosing spondylitis. Many studies also suggest biologics help prevent progression of spinal fusion especially in high-risk patients.
Non-medication treatments and practices that may help are physical therapy, physical activity, quitting smoking, and managing your diet and stress.
- Research has found that people with AS who smoke have more spinal damage than non-smokers. Smoking can worsen the pain of AS and impact how well medication like biologics work.
- A physical therapist can develop an individualized program designed to help you increase your strength, flexibility, range-of-motion, and general mobility and exercise tolerance through a wide variety of therapeutic treatments and strategies.
- Physical activity can help manage pain and stiffness. Getting regular movement in the joints can help manage the symptoms of the disease and help people living with AS maintain their flexibility and mobility.
- It is important to maintain a weight that is healthy for you; being overweight can place stress on joints, which may worsen symptoms of AS. The anti-inflammatory diet may reduce symptoms in some people.
- Stress can worsen symptoms like inflammation and chronic pain. Ways to manage stress include, but are not limited to, meditation, going to support groups, counselling, breathing exercises, massage, and being in nature.
To learn more about ankylosing spondylitis, please visit Arthritis Consumer Experts’ disease spotlight on ankylosing spondylitis here.